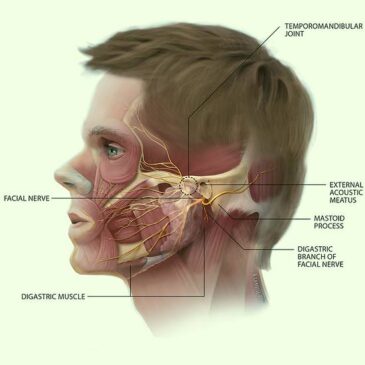
Causes & Symptoms
The incidence of TMJ disorders is higher in women than men, although not strikingly. Whilst age brings certain causes such as arthritis, cases in middle age are higher.
Interference can come from a mild condition, called temporomandibular joint dysfunction, which often improves with rest and lifestyle changes. TMJ treatment may still be required, depending on natural progress.
A range of conditions can be more serious. Dislocation, or other abnormal relationships between the disc and articular surfaces are common, which can be due to tooth grinding, or clenching, or overloading your jaw muscles.
External trauma, including fractures, can reduce the joint’s function. Inflammation can arise from a number of medical conditions or be related to arthritis such as rheumatoid arthritis, or degenerative osteoarthritis.
TMJ disorder is likely to be unpleasant, with pain in the muscles, jaw joint, face, or neck. Jaw stiffness, or restricted movement and clicking, or popping sounds are common. Occasionally there may be joint swelling.
Although natural misalignment is not usually a root cause, how your upper and lower teeth come together can change due to joint dysfunction. Headaches, hearing loss, or tinnitus are other common side effects.
The causes of temporomandibular joint problems can be multi-factorial. Accurate assessment is critical for successful treatment to eliminate symptoms.
Professional Diagnosis
Our specialist maxillofacial consultant will carry out a detailed oral examination. Panoramic X-Rays, or other specialist imaging techniques may be required, to define the detail of your jaw, joints and surrounding soft tissues.
Your medical history, including any relevant family medical history might be discussed, as genetic factors can have a relationship with TMJ disorder.
Issues such as mouth sores, gum disease, sinus function, or unexplained toothache will be investigated as will previous trauma to the face, or jaw, including biting hard, or unusually wide mouth opening.
Your jaw joints and nearby areas can be examined for pain, clicking, popping, or grating, and your bite and facial muscle function will be analysed during a consultation.
Jaw problems can create stress, tension, headaches, or pain which transfers into your shoulders. Each are symptoms which deserve investigation and are quite common in relation to TMJ disorders.
For such a vital function, examining multiple potential causes will help to ensure that decisions on treatment are the right ones for you.
A Range Of Treatment
Developing a Personalised Treatment Plan
Your clinical assessment including examination findings, imaging results if carried out and your consultant’s expertise will contribute to creating a precise treatment plan. The ethos of our clinic is to minimise surgery, we tend to manage TMJ symptoms conservatively.
Non-Surgical Approaches
Relaxation techniques can assist, as can dietary changes, or jaw joint physiotherapy. Stopping jaw clenching, grinding, or nail biting can address the problem. A clear plastic splint is available to fit over your teeth, worn at night, to support the temporomandibular joints and decrease grinding.
A procedure called Occlusal Equilibration can be used with gentle reshaping of the biting surfaces of individual teeth, to create a more even bite. Other dental work can achieve bite balance, such as replacing missing teeth.
Antidepressant medication may assist, not simply because psychological factors could be involved, the medication has a muscle relaxing and pain killing effect.
Minimally Invasive Surgical Options
Surgery is available but only in a small proportion of cases. This ranges from simple steroid injections into the joint, washing the joint out with sterile fluid, eliminating tissue adhesion, or dislodging a stuck cartilage disc.
When Major Surgery is Necessary
Significant open joint surgery is rarer. This may be indicated if bones within the jaw joint are notably deteriorating, a tumour is found to be a cause, or severe scarring, or bone chips lay inside the joint.
Surgery can include replacing the joint with a modern implant, to be considered where damage, injury, arthritis, infection, or pain cannot be solved in other ways.
Your consultant will counsel you on any procedure that may be needed and discuss this thoroughly. Even in expert hands, open joint surgery brings a greater healing time and some possibility of nerve injury.
Care At Our London Clinic
Seeing a leading maxillofacial consultant is a critical first step in assessing and managing TMJ conditions to ensure the right treatment plan is put in place.
Where a TMJ disorder is the primary issue, your treatment will focus on minimum intervention for maximum effect. A high level of care should be based on full recovery, without unnecessary risks.
We appreciate the loss of function and the pain that TMJ disorders can bring as well as the impact on core activities such as eating, or speaking. Our team is here to help get you back to normal function as quickly as possible.